Urine Leakage
What Is Incontinence?
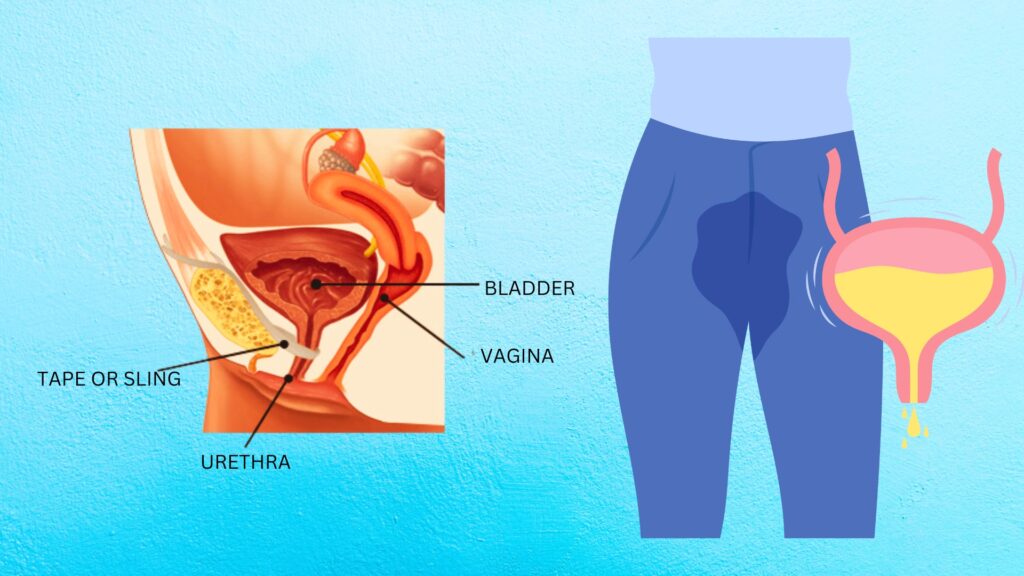
Urinary incontinence is when you lose control of your bladder and leak pee. It’s a condition that can have a negative effect on your life.
Your urinary system consists of many different organs. These organs work together to filter, store and remove waste from your body as pee (urine). When your urinary system works as expected, you usually have time to get to a bathroom to pee, and you don’t leak pee. Urinary incontinence occurs when these parts don’t operate as they should. This can happen for many different reasons throughout your life.
Many people think incontinence is a normal part of getting older, and you can’t do anything to stop it. It’s true that your risk of incontinence increases as you get older. But it can happen to anyone, regardless of age. And treatments are available to help you manage it. Incontinence doesn’t have to disrupt your life or keep you from being active.
Urinary incontinence is very common. About 62% of females age 20 and older have some type of urinary incontinence. In males, a little less than 14% have incontinence.
Symptoms and Causes
Urinary incontinence is the involuntary leakage of urine, often happening before reaching the bathroom or during activities like sneezing, laughing, or exercising. Symptoms can vary from a constant drip to occasional leaks. Common signs include:
Frequent urination (more than eight times a day)
Needing to urinate but passing only small amounts
Waking up more than twice at night to urinate (nocturia)
Wetting the bed (enuresis)
Leakage during physical activities or sexual intercourse
Causes vary by gender and can be temporary or chronic. Temporary causes include urinary tract infections, pregnancy, medications (diuretics, antidepressants), caffeine, alcohol, and constipation. Chronic causes include overactive bladder, stroke, diabetes, menopause, multiple sclerosis, Parkinson’s disease, enlarged prostate, and prostate surgery.
Pregnancy causes incontinence by putting pressure on the bladder and weakening pelvic floor muscles. Women are more prone due to childbirth and hormonal changes during menopause. Older age also increases risk.
Managing incontinence with a healthcare provider can help improve quality of life.
Diagnosis and Tests
A healthcare provider diagnoses urinary incontinence by reviewing symptoms, medical history, and performing a physical exam. Key questions include how often you urinate, frequency and amount of leakage, onset of symptoms, medication use, pregnancy, and childbirth history. These help identify leakage patterns and incontinence types.
Diagnostic tests may include:
Pelvic exam to assess muscle strength and rule out other causes.
Digital rectal exam to check for an enlarged prostate.
Urinalysis to detect infections or blood in urine.
Bladder ultrasound to evaluate bladder function and emptying.
Stress test where you perform activities to observe leakage.
Cystoscopy to examine the urethra and bladder internally.
Urodynamic tests to measure bladder capacity, pressure, and flow.
Pad test to quantify urine leakage.
Keeping a bladder diary noting urination frequency, leakage, and triggers aids diagnosis and treatment planning.
Treatment Options
Urinary incontinence treatment depends on your specific type and comfort level. Main treatment options include:
Lifestyle changes: Timed voiding, peeing before activities, avoiding heavy lifting, Kegel exercises, limiting fluids before activities, wearing absorbent pads, bladder retraining, maintaining a healthy weight, and vaginal inserts to support the urethra.
Medications: Drugs like oxybutynin, tolterodine, solifenacin, fesoterodine, darifenacin, trospium, mirabegron, and vibegron can either calm bladder contractions or relax muscles. Vaginal estrogen may be prescribed in menopause to restore bladder function.
Procedures and surgery: Options include bulking agents to thicken the urethral lining, Botox injections to relax bladder muscles, neuromodulation devices to stimulate nerves, sling procedures to support the urethra, and artificial urinary sphincters especially after prostate cancer surgery.
Providers tailor treatment plans based on symptoms, type of incontinence, and individual needs.
Prevention Strategies
Preventing all types of urinary incontinence isn’t always possible, but you can reduce your risk by:
Keeping pelvic floor muscles strong with regular Kegel exercises
Maintaining a healthy body weight to lessen pressure on the bladder
Drinking the right amount of fluids at the right times and avoiding bladder irritants like caffeine and alcohol
Avoiding constipation by eating a high-fiber diet and staying hydrated
Quitting smoking to prevent coughing that weakens pelvic muscles and bladder irritation
Practicing good bladder habits, like going to the bathroom when needed and fully emptying your bladder
Living with incontinence may cause stress, anxiety, or depression. Talking to a therapist or psychologist can help manage these feelings.
See a healthcare provider when you first notice symptoms to get the right diagnosis and treatment options.
Ask about your type of incontinence, recommended treatments, and possible side effects.

